
Glaucoma
Glaucoma
Don't Let Glaucoma Steal Your Eyesight
Glaucoma is an eye disease that damages the optic nerve, which connects the eyes to the brain. The optic nerve is responsible for sending electrical impulses to the brain, which the brain then interprets. Often, glaucoma is caused by high intraocular pressure, or pressure inside the eyes.
Schedule a consultation with us today to get a thorough evaluation from our New York glaucoma specialist. Save your vision now before it’s too late.

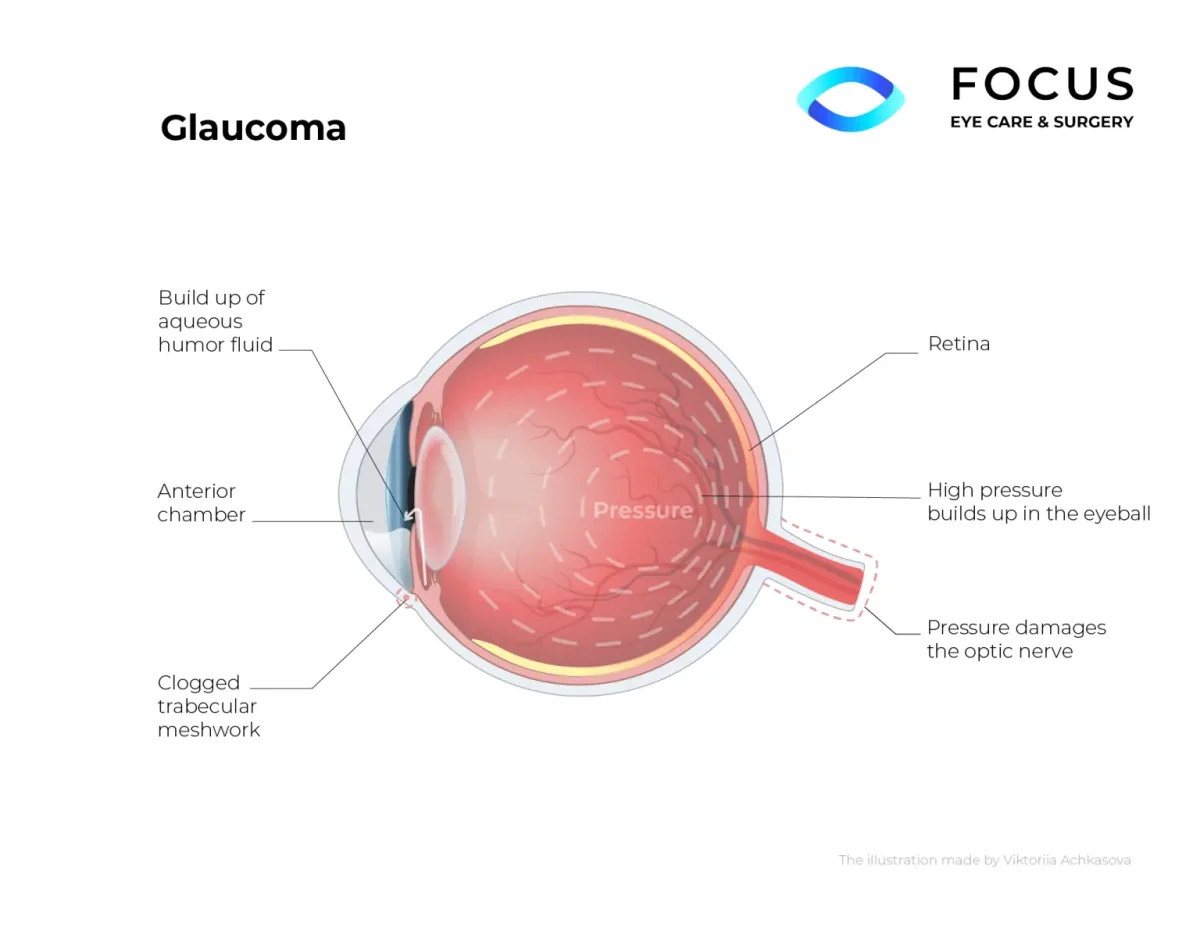

You may be going blind and not know it.
This is what happens when you have glaucoma, which eye doctors call the ‘silent thief of sight.’ Because it’s stealthy, glaucoma is one of the leading causes of vision loss in the United States and around the world. Sometimes, significant damage has already taken place before it is even noticed.
This is why getting regular, comprehensive eye exams is crucial to detect the disease early on and get treatment before further vision loss happens. At Focus Eye Care & Surgery, our New York eye specialist, Dr. Neelofar Ghaznawi, is board-certified to provide medical and surgical treatments to specialized ophthalmic conditions.
If you suspect you have glaucoma, schedule a comprehensive dilated eye exam with us today so you can take action early and save your vision.
What Are the Symptoms of Glaucoma?
In its early stages, there are no warning signs of a developing glaucoma. Only later when the disease has progressed you may start to notice:
- Gradual loss of peripheral vision, as if looking through a tunnel
- Blurred vision
- Colored rings around lights
If glaucoma does develop suddenly, you may see or feel:
- A headache
- Red eyes
- Tenderness around the eye area
- Severe eye pain
- Nausea and vomiting
- Colored rings around lights
This sudden onset of symptoms may signal an acute attack, which requires emergency care to prevent blindness.
At present, loss of vision due to glaucoma is not reversible. But with prompt detection and treatment, vision can be saved or further vision loss can be avoided.

How Do You Know If You Have Glaucoma?
The only way to find out if you have glaucoma is to get a comprehensive dilated eye exam.
The eye doctor will look through your wide open eyes with a special instrument to examine the health of the optic nerve. When there is damage, the cupping (depression in the middle) of the optic nerve when viewed from the front of the eyes is enlarged due to high intraocular pressure.
FAQs About Glaucoma
The intraocular pressure (IOP) is the pressure inside the eyes. For the eye to maintain its globular shape, the IOP should range somewhere from 10–21 mm Hg.
It is possible, however, to have IOP higher than normal and not experience any injury to the optic nerve. Conversely, it is possible to have IOP lower than the rest of the population and sustain damage to the optic nerve. This is because some people have sensitive optic nerves susceptible to any slight increase in IOP.
Normal IOP is maintained by the equal secretion and outflow of aqueous humor. This clear, watery fluid is secreted by the ciliary body located between the iris, the colored part of the eyes, and the natural lens just behind it. Aside from maintaining pressure within the eye, the aqueous humor nourishes and cleanses the lens.
In a normal eye, the fluid flows out of the pupil, the opening of the iris. It then drains out of the trabecular meshwork, a porous channel in the sides of the cornea. The cornea is the clear, dome-shaped surface layer of the eyes.
Finally, the aqueous humor collects in the Schlemm’s canal before it exits via the episcleral veins, and out into the body.
Any obstruction in this process causes fluid to build up, pressing onto the lens, which in turn, presses onto the optic nerve.
In glaucoma, the angle refers to the meeting point between the cornea and iris. The most common types of glaucoma are:
Open-angle glaucoma
In open-angle glaucoma, the angle is wide open without obstructions. Fluid backs up because of clogged trabecular meshwork or episcleral veins. Over time, this buildup increases the IOP.
The trabecular meshwork may not drain properly due to certain diseases, such as scleritis, or inflammation of the sclera, the white portion of the eye.
Protrusion of the eyeballs secondary to a hyperactive thyroid (exophthalmic goiter) may also block the episcleral veins even as the trabecular meshwork drains well.
Narrow-angle glaucoma
In this type of glaucoma, the angle is narrow and sometimes even closed; hence the alternate name ‘angle-closure’ glaucoma. This could be because when the iris dilates, it presses too close to the cornea. As there is no way for fluid to drain out of the eyes, it builds up and leads to high IOP.
Normal pressure glaucoma
Intraocular pressure is within normal range and yet there is damage to the optic nerve. This could be because the nerve is susceptible to even slight increases in IOP.
Depending on the severity of your glaucoma, your treatment may include oral medications, prescription eyedrops, conventional surgery, or laser surgery.
At Focus Eye Care & Surgery, our eye surgeon in New York uses the latest surgical techniques and cutting-edge laser technology to perform FDA-approved laser glaucoma surgery in an office setting.
Selective Laser Trabeculoplasty (SLT) – laser is focused to the eyes through a contact lens to initiate a change in the eye structure that declogs or exposes the trabecular meshwork. Eye surgeons often use this technique as a first line treatment for open-angle and normal pressure glaucoma.
Laser Peripheral Iridotomy (LPI) – laser is focused to the edge of the iris to create a pinprick hole where the aqueous humor can seep out. As the pressure behind the iris lowers, the angle opens up, allowing the fluid to drain properly. This laser technique is typically used to treat and prevent acute attacks of narrow-angle glaucoma.
The major risk factors of glaucoma are: Age over 60 years, Family history of glaucoma, Diabetes and high blood pressure, African American race, Eye tumors, inflammation, or other eye disorders.
Glaucoma is diagnosed by a series of eye tests including tonometry to measure eye pressure, visual acuity measurement, visual field tests, pachymetry to measure corneal thickness, and other supplementary tests. A diagnosis of glaucoma can be made if intraocular pressure is above 20mm Hg and visual field defects are found to have already occurred.
Studies have found that drinking water can temporarily raise the pressure in the eyes, but this pressure also lowered quickly to baseline levels. It is unlikely that drinking water can worsen glaucoma, but experts recommend that water should be drunk in smaller quantities more frequently throughout the day than to drink a large volume of water at once to avoid sudden rises in eye pressure.
In the early stages of open-angle glaucoma, most people experience no symptoms at all. As glaucoma progresses, you may notice blurring of vision or halos. However, in acute angle-closure glaucoma, symptoms such as severe headache, eye pain, nausea, and vomiting can occur early on. Acute angle-closure glaucoma is an emergency condition that requires prompt treatment.
Yes, sleep positions can change eye pressures. Studies have found that sleeping itself can elevate the pressure in your eyes. Sleeping on your side or on your back does not raise intraocular pressure by much, but sleeping on your stomach with your head down can significantly increase the intraocular pressure.
Regular aerobic exercises such as jogging and brisk walking can be beneficial to lower intraocular pressure in patients with glaucoma. But, strength training exercises can increase intraocular pressure from muscle exertion and may worsen glaucoma.
Although glaucoma cannot be cured, various treatment options exist to manage and halt glaucoma progression. Glaucoma can be treated by medication that lowers the intraocular pressure by either increasing the outflow of aqueous humor, which is the fluid within your eyes, or by decreasing aqueous humor production. These medications can be in the form of eye drops or oral drugs. Laser surgery that widens or opens the outflow tract for aqueous humor can also be done to treat glaucoma.
Foods rich in vitamins such as kale, cabbage, celery, carrots, beets, and peaches can reduce the risk of developing glaucoma. Once glaucoma has developed, a healthy diet, exercise, and adherence to treatment may be helpful to prevent glaucoma from worsening.


Are You a Candidate for
Vision Correction?
Whether you just need a general eye exam, or if you are interested in reducing or eliminating your need for glasses or contacts, our team is here to help! Contact us to book an appointment today!
The doctors at Focus Eye Care & Surgery have reviewed and approved this content.
Page Updated:


