
Diabetic Macular Edema
Diabetic Macular Edema
Diabetic Macular Edema Could Result in Irreversible Blindness
Damage to the small blood vessels in the retina is a common complication of diabetes. According to the National Eye Institute, of the 7.7 million Americans who have diabetic retinopathy, almost 10% have diabetic macular edema, which could result to irreversible blindness if left untreated.
Diabetic macular edema is most noticeable when it has already advanced to cause significant visual impairment. Because of the silent nature of the disease, it is critical to undergo regular, comprehensive eye exams to save the remaining vision and stop further vision loss.
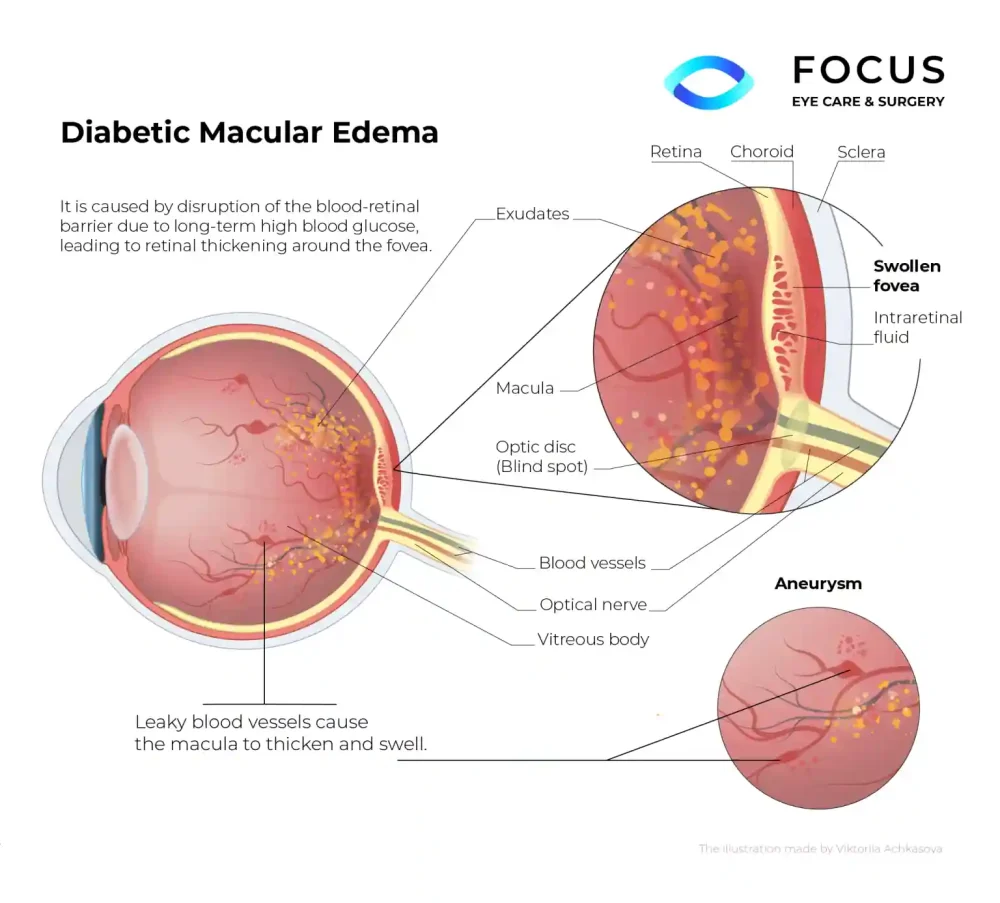
Worried That Diabetic Macular Edema Would Steal Your Eyesight?
Schedule a consultation with us today. Our New York eye specialist will develop a treatment plan with you to address your individual needs, so you enjoy enhanced quality of life.
At Focus Eye Care & Surgery, our board-certified New York eye specialist, Dr. Neelofar Ghaznawi, uses state-of-the-art equipment to perform comprehensive eye exams. The result is accurate diagnosis used to develop a personalized treatment plan with you that best suits your goals and needs. Dr. Ghaznawi is a member of the American Academy of Ophthalmology.
FAQs About Diabetic Macular Edema
Macular edema is the buildup of fluid (edema) in the macula, the part of the retina responsible for sharp, central vision.
Diabetic macular edema is a serious complication of diabetic retinopathy. Blood vessels in the retina, the light-sensitive tissue lining the back of the eyes, are damaged due to uncontrolled high blood sugar levels.
Early signs of DME are not noticeable, especially if only one eye is affected. Over time, swelling of the surrounding retinal tissues results in:
- Blurred vision
- Colors looking washed out
- Wavy vision near the center of the visual field
Without treatment, DME can cause detachment of the retina or permanent blindness.
The most effective way to slow the progression of DME remains blood sugar control and management of diabetes-induced systemic symptoms. This includes controlling high blood sugar and fluid retention due to kidney damage.
If DME has advanced to a stage where it threatens significant visual impairment, the following procedures may help save and even improve the remaining vision:
Anti-VEGF injectable
Medications that reduce edema and slow down growth of new abnormal blood vessels in the retina are delivered into the eye using a thin needle. They are called anti-angiogenic drugs that contain anti-vascular endothelial growth factor.
Anti-VEGF medications have become the first line of treatment for people with DME. Potential risks include adverse effects to the body’s blood vessels resulting in stroke and heart attack.
Laser photocoagulation
Laser photocoagulation involves focusing a high energy laser beam onto leaking blood vessels in the retina (avoiding the macula). The goal is to seal them off and prevent growth of new problematic blood vessels.
If the leak is located close to the macula, residual blurring of central vision may be expected. For some people, retreatment may have to be done in 3 to 5 years for the therapy to be effective.
People with diabetic retinopathy (DR) have an increased risk of developing DME. Because most people with diabetes experience DR to some degree, it is critical to control diabetes before it causes complications affecting vision.
Diabetic macular edema may present without any symptoms in the early stages. If you notice symptoms such as central vision blurriness or wavy appearance, washed-out appearance of colors, and difficulties with reading, then this could indicate that the blood vessels in your eye are leaking. When you notice these symptoms, you must visit your ophthalmologist as soon as possible to prevent blindness.
Various treatment options are present to manage and prevent macular edema from progressing to blindness. The most important treatment measure is to control the underlying cause of macular edema such as diabetes and high blood pressure. Other treatments targeted at treating macular edema include anti-VEGF injections, steroid eye drops, vitrectomy, and laser treatment.
No, diabetic macular edema does not resolve on its own. Appropriate and prompt measures must be taken to prevent diabetic macular edema from worsening and impairing vision.
Yes, diabetic macular edema is a serious issue as it can lead to blindness and disability if early treatment is not started.
Drinking large volumes of water can temporarily increase intraocular pressure. Macular edema can lead to complications such as glaucoma, which may be worsened by any further rise in intraocular pressure.
How can diabetic macular edema be treated? The most important step to treat macular edema is managing the underlying cause responsible for macular edema such as diabetes and high blood pressure. Blood glucose levels and blood pressure should be within the normal range to prevent further worsening of macular edema. Other treatment options targeted at treating macular edema include: Anti-VEGF injections directly into the vitreous cavity to stop the proliferation of small blood vessels that can easily rupture and cause macular edema; Steroid eye-drops can also be used to control inflammation; Vitrectomy is an outpatient surgical procedure that is done to remove the strain on the retina due to pulling forces from the vitreous; Laser to coagulate bleeding vessels is also a treatment option but is rarely performed.
Yes, diabetic macular edema can severely damage central vision and can even progress to blindness if not treated immediately.
No, all macular edemas are not caused by diabetes. The most common cause of macular edema is diabetes-induced retinopathy, but other causes can include high blood pressure, age-related macular degeneration, retinal vein occlusion, vitreomacular traction, retinitis pigmentosa, inflammatory eye disease, eye tumors, past eye surgery, and injuries.


Are You a Candidate for
Vision Correction?
Whether you just need a general eye exam, or if you are interested in reducing or eliminating your need for glasses or contacts, our team is here to help! Contact us to book an appointment today!
The doctors at Focus Eye Care & Surgery have reviewed and approved this content.
Page Updated:


